Table of contents
Bartonella false positives are common
In chronic Lyme pseudoscience groups, patients are often misled into believing they have multiple fake diagnoses, not just “chronic Lyme”. Quite commonly, patients desperate for an explanation to their symptoms receive false diagnoses of “chronic Bartonella.”
Bartonella is a genus of bacteria, and the most common species transmitted to humans in North America is called Bartonella henselae. As discussed in more detail below, Bartonella henselae causes cat-scratch disease, which clears up on its own in most cases and results in lifelong immunity.
The CDC debunks some common myths about Bartonella:
- “There is no evidence that ticks spread Bartonella infection to people.” (source)
- “Unfortunately there is a great deal of misinformation regarding multiple tickborne infections (called coinfections) on the internet. The possibility of having several tickborne infections at once or having pathogens such as Bartonella that have not been shown to be tickborne, is extremely unlikely.” (source)
A 2024 European review states:
The microbe has been detected in ticks in Europe but transmission of infection to humans by tick bites has not been demonstrated. Routine testing for this pathogen after tick-bites is not currently recommended.
A 2024 CDC study found no Bartonella in 1641 blacklegged ticks collected from across the US. An August 21, 2024 search of the TickReport database revealed zero positive results in 13.16k ticks tested for Bartonella.
Since Lyme bacteria (Borrelia burgdorferi) is only spread by black legged (Ixodes) ticks and Bartonella is not a known tick-borne infection in the United States or Europe, Bartonella is not a coinfection of Lyme disease.
Bartonella is also not a coinfection of Babesia, an infection that is spread by the same tick as Lyme disease in the northeast United States.
“Lyme literate” doctors: misinformation and fraud
Unfortunately, false claims of multiple coinfections are made by quacks and their patients. Often, the quacks and hopeful patients are well-meaning but simply wrong.
Quacks may demonstrate red flags such as using deceptive marketing terms like “Lyme literate”, integrative, functional, alternative, and naturopathic. They also may spread conspiracy theories about mainstream medicine in order to distract from their mistreatment of patients.
Carol Ryser, MD was a “Lyme literate” felon who was sued by numerous patients who she abused. The story of Ryser’s patient Andrea Ratliff is particularly horrific. According to Ratliff’s lawsuit:
- A nurse at Ryser’s clinic, Diana Gordon (formerly Diana Smith), recorded that Andrea had 20 different disorders, including Lyme disease and heavy metal toxicity.
- “Smith told Andrea Ratliff to start taking multiple medications and supplements, to alter her diet, and to begin medical and alternative treatments to address the conditions Smith had recorded in the medical record.”
- Ryser diagnosed Ratliff with “Lyme disease, Borrelia burgdorferi, bartonella, babesia, tick borne encephalitis, hypercoagulation, beta strep, hyperthyroidism, immunoglobulin deficiency, migraine, chronic fatigue syndrome, Levitor reticularis [sic], and other conditions.”
- “Andrea Ratliff rapidly gained weight during treatment and showed Ryser stretch marks that had appeared on her skin. Ryser told her that the stretch marks were not in fact stretch marks but were actually ‘bartonella’ ‘becoming active.'”
- “During the course of treatment, Ryser additionally diagnosed Andrea with ehrlichiosis, Rocky Mountain spotted fever, coxsackie virus, anaplasma, influenza, and other infectious diseases, with the explanation that these ‘bugs’ had been in her body for years but were surfacing because of Ryser’s treatment.”
- “Despite Andrea’s increasing sickness during the treatment, Ryser told the Ratliffs that they had some infections ‘running for the hills.’ Ryser told Andrea and Tadd that the bartonella was ‘trying to get away’ in her body and that was making her feel ‘sicker.'”
- Ryser’s clinic treated Ratliff for 6 months with IV antibiotics and prescribed “other treatments, oral medications, simultaneous oral antibiotics, supplements, diets, and painful injections for years.”
The assessments of Ryser and Gordon were bogus. As seen in Ratliff’s story, pseudoscience advocates falsely claim that harmless stretch marks are a “bartonella rash” or “bartonella tracks”.
The “Lyme literate” are notorious for concocting false stories in order to justify fake diagnoses and extreme treatments. The abuse is both physical, from the unnecessary treatments, and psychological, from the unnecessary anxiety generated about “bugs” and “biofilms”.
In a 2013 survey by quackery propaganda group LymeDisease.org, 54% of respondents claiming to have chronic Lyme disease—itself an unrecognized diagnosis— also claimed to have a Bartonella coinfection. As detailed in our post on tick-borne infections in the United States, the survey results defy reality.
But what about positive tests?
Confusion may be caused by inappropriate use of testing. Many people produce antibodies to Bartonella bacteria, but this does not mean that Bartonella is causing symptoms.
In a study of Italian children, 62% had antibodies to Bartonella but no evidence of cat-scratch disease. Another study found 30% of Germans produce antibodies to Bartonella.
A 2021 Swedish study attempted to determine if there was a plausible hidden epidemic of bartonellosis symptoms, but didn’t find one. Looking antibody testing in blood serum (serology), the study authors concluded:
Positive Bartonella serology was not linked to any specific symptom, nor to (suspected) tick-bite exposure.
Dubious DNA tests
In addition, CDC scientists have called into question certain PCR (DNA) tests that have not been validated. The scientists criticized one paper by fringe researchers Edward Breitschwerdt, Ricardo Maggi, Bobak Robert Mozayeni, Elizabeth Pultorak, Barbara Hegarty, Julie Bradley, and Maria Correa, as containing “serious flaws in content and underlying message.”
The Breitschwerdt paper inexplicably claimed many subjects tested positive for Bartonella DNA by PCR and yet did not test positive for Bartonella antibodies. Since a Bartonella infection typically provokes an immune response, the scientists questioned the contradictory and implausible results.
Profits over ethics?
Breitschwerdt, Maggi, and Mozayeni became executives in the for-profit company Galaxy Diagnostics, which sells expensive testing for Bartonella and tick-borne diseases. They stand to profit from disease mongering about Bartonella and other infections they peddle tests for.
In addition to selling questionable bartonella testing, Galaxy also advertises dubious urine tests purported to detect Lyme disease using “Nanotrap” technology. As illustrated by the IgeneX urine test debacle, urine testing for Lyme disease has a bad history. Experts recommend against urine tests for Lyme.
Breitschwerdt and Maggi are employees of the College of Veterinary Medicine at North Carolina State University, which sadly provides them an air of credibility.
Mozayeni, a medical doctor, is a former president of the pseudoscience group ILADS (International Lyme and Associated Diseases Society). Mozayeni and Breitschwerdt were listed as speakers at an ILADS conference. In 2010, the Healthcare Protection Agency of UK issued scathing conclusions about guidelines issued by ILADS:
- The ILADS guidelines are not evidence-based and are poorly constructed.
- Application of the ILADS guidelines’ poorly defined case definitions will result in a very high risk of misdiagnosis.
- Use of ILADS guidelines’ vague treatment recommendations, including prolonged use of antibiotics, has potentially serious consequences.
- Patients misdiagnosed with Lyme disease risk losing opportunities for diagnosis and treatment of other conditions. They also risk serious physical, psychological social and financial adverse events.
Mozayeni runs the shady companies Translational Medicine Group, Bethesda Hyperbaric Oxygen Therapy, and T Lab, which are located in Bethesda, Maryland. The subjects of the Breitschwerdt paper discussed above were patients examined and selected by Mozayeni.
Doctors are very concerned about patients who have been diagnosed with false Bartonella infections because the patients may receive unnecessary treatments and delay treatment for a real conditions. Ultimately, a positive test is not necessarily meaningful. Because of the confusion surrounding testing, the CDC advises:
It is important for all abnormal test results to be interpreted with your health care provider in the context of your medical history.
Beware of predatory labs
The CDC has explained that there are no FDA-cleared tests for Bartonella on the market. Sadly, disreputable and expensive labs have popped up that are used to facilitate false diagnoses.
Using IgeneX and other labs associated with “Lyme literate” charlatans as an example, the FDA has warned about lab-developed tests, which have little regulatory scrutiny.
LymeScience recommends against patronizing the following labs: Galaxy Diagnostics, IgeneX, BCA Lab (also called InfectoLab), DNA Connexions, T Lab Inc (aka TLab), ArminLabs, Vibrant America/Vibrant Wellness, Medical Diagnostic Laboratories (MDL), and others listed on our Red Flags of Chronic Lyme Quackery page.
Fake Bartonella photos flood the Internet
Cat-scratch disease is caused by infection with bacteria called Bartonella henselae. According to the CDC, typical symptoms include:
- Low-grade fever may be present
- Enlarged, tender lymph nodes that develop 1–3 weeks after exposure
- A papule or pustule at the inoculation site
This is a photo of real papules caused by Cat-scratch disease:
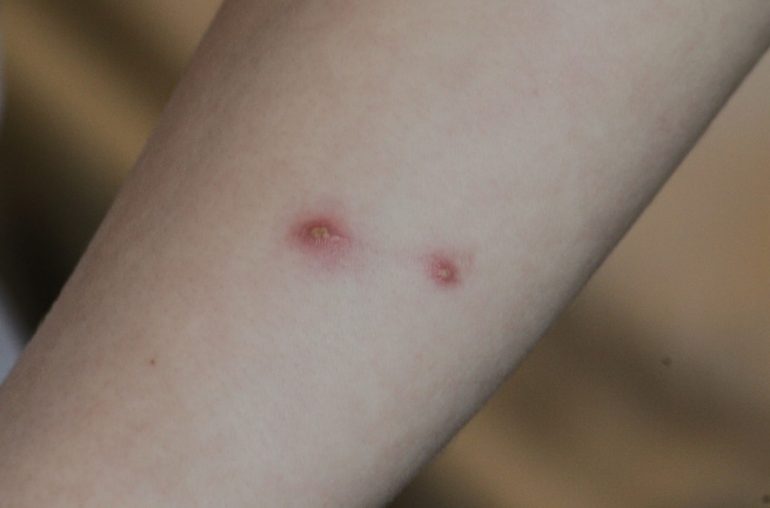
In chronic Lyme groups, dubious photos of rashes are commonly presented as evidence of Bartonella infection. In reality, these photos are typically stretch marks, a common skin condition also called Striae distensae. Stretch marks associated with pregnancy are called striae gravidarum.
According to Medscape:
- Approximately 90% of pregnant women, 70% of adolescent females, and 40% of adolescent males (many of whom participate in sports) have stretch marks.
- Prolonged use of oral or topical corticosteroids or Cushing syndrome (increased adrenal cortical activity) leads to the development of striae.
Actress Jameela Jamil has proposed renaming stretch marks to “Babe Marks” while Chrissy Teigen calls them “stretchies.”
Below is a photo of typical stretch marks:
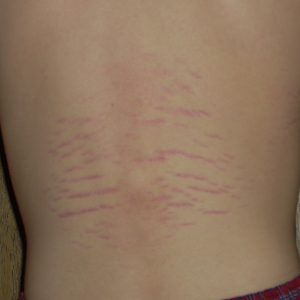
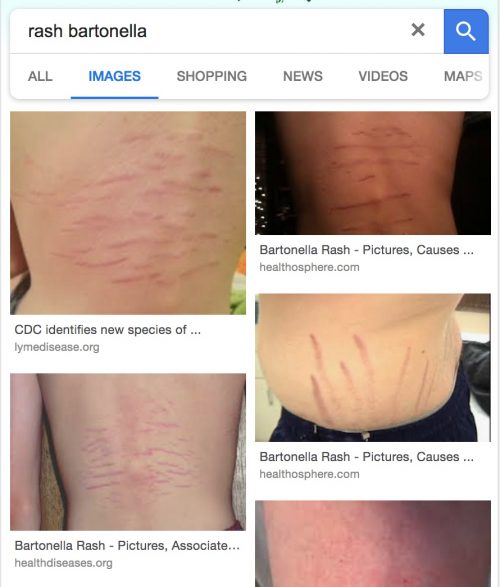
As shown below, a search for “rash bartonella” on Google Images returns photos that are likely stretch marks and not skin manifestations of Bartonella. The top hit is from the pseudoscience organization LymeDisease.org.
No reputable science organization features photos like this of Bartonella. One of the images is just a mislabeled version of the Wikimedia stretch marks image.
Dermatologists reassure the public
⭐ More: Full study from Johns Hopkins
Upon discovery, stretch marks can seem concerning to parents and teenagers. Fortunately, scientists in the Department of Dermatology at Johns Hopkins University studied the issue in 2018 by reviewing cases of horizontal stretch marks observed on the lower backs of teenage boys.
The scientists found that horizontal stretch marks of the lower back:
- have nothing to do with bacterial infection, including Bartonella or Borrelia burgdorferi, the cause of Lyme disease.
- are associated with rapid growth spurt, tall stature, and family history of stretch marks.
- are not related to chronic medical conditions or anabolic steroid use.
- do not warrant any further medical testing.
Additionally, the scientists reviewed the literature and found no compelling scientific evidence of a link between any stretch marks and infection with Bartonella henselae or Borrelia burgdorferi. They noted that unsubstantiated information spread by Lyme-oriented web sites (such as LymeDisease.org, LymeActionNetwork.org, and LymenetEurope.org) may cause unnecessary concerns from parents.
The American Academy of Dermatology has more information on why stretch marks appear and how to get rid of them.
What is real Bartonella?
Several Bartonella species are known to infect humans. Bartonella henselae causes cat-scratch disease because the bacteria is transmitted to humans from a scratch of a cat.
As stated above, cat-scratch disease often causes enlarged lymph nodes (lymphadenopathy), typically in the underarm, head/neck, or groin. This is photo of a 5-year old child with lymph node growth in the underarm due to cat-scratch disease:
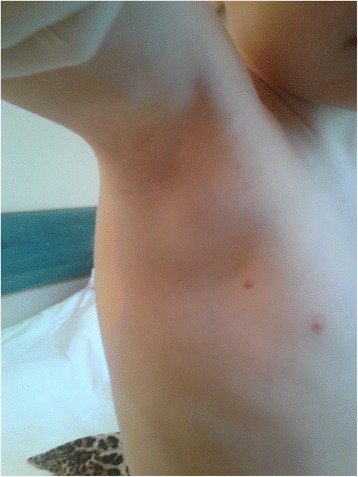
Lymph node growth occurs in many different conditions, so this symptom alone cannot be used to diagnose cat-scratch disease.
Trench fever: A severe disease often related to homelessness
The human body louse (lice) transmits Bartonella quintana to humans, causing Trench fever. The National Organization for Rare Disorders states that Trench fever “is commonly found in homeless, alcoholic, and poverty-stricken populations where poor sanitation and poor hygiene often occurs.”
CDC has reported on the harms of Bartonella quintana to homeless individuals.
Bartonella treatments
Cat-Scratch Disease treatments
Most cases of cat-scratch disease go away on their own, so antibiotics are typically not recommended. Instead, guidelines recommend analgesics and careful monitoring. Though there is little data to support specific antibiotic treatment of cat-scratch disease in patients with functioning immune systems, antibiotics (e.g. a 4 day course) are sometimes used in complicated cases.
A very small subset of patients, such as the immunocompromised, may develop worse symptoms and require special treatment. For example, cat-scratch disease and other Bartonella infections can be more serious in HIV/AIDS patients or those receiving immunosuppressant drugs. Bartonella has also been recognized as causing of neuroretinitis and endocarditis, severe manifestations.
According to infectious disease specialist Dr. Katarzyna Mazur-Melewska and colleagues:
One episode of cat-scratch disease confers lifelong immunity to all patients.
Other Bartonella species treatments
For Trench fever and serious complications of Bartonella, the CDC recommends consulting with an infectious disease expert and treating with antibiotics.
Herbs for Bartonella?
Like for Lyme disease, there is no scientific evidence to support herbs and supplements to treat Bartonella.
See also: Why herbs and supplements aren’t recommended for Lyme disease
We encourage consumers to run far away from unscientific practitioners who profit from sales of herbs and supplements.
Conclusion
Given the known characteristics of Bartonella, the claims of chronic tick-borne Bartonella infections are simply not supported by science. A real Bartonella infection bears little resemblance to how it is portrayed in non-science-based forums online.
Despite claims by chronic Lyme activists of numerous chronic tick-borne coinfections, a 2014 scientific review concluded:
The medical literature does not support the diagnosis of chronic, atypical tick-borne coinfections in patients with chronic, nonspecific illnesses.
In other words, the diagnoses of chronic coinfections that chronic Lyme advocates have received are likely misdiagnoses.
Resources
- CDC: Bartonella site index (archive)
- American Academy of Family Physicians: Cat-Scratch Disease
- Dr. Warren Heymann: Striae Due to Bartonella is a Stretch
- Bartonella Treatment Guidelines: Angelakis E, Raoult D. Pathogenicity and treatment of Bartonella infections. Int J Antimicrob Agents. 2014. (mirror)
- Rolain JM, et al. Recommendations for treatment of human infections caused by Bartonella species. Antimicrob Agents Chemother. 2004.
- Lantos PM, Wormser GP. Chronic coinfections in patients diagnosed with chronic lyme disease: a systematic review. Am J Med. 2014;127(11):1105-10. [Discusses dubious diagnoses of Bartonella, Anaplasmosis, and Babesia]
- Wormser GP, Pritt B. Update and Commentary on Four Emerging Tick-Borne Infections: Ehrlichia muris-like Agent, Borrelia miyamotoi, Deer Tick Virus, Heartland Virus, and Whether Ticks Play a Role in Transmission of Bartonella henselae. Infect Dis Clin North Am. 2015.
- CDC scientists complain about misinformation on Bartonella
- Telford SR, Wormser GP. Bartonella spp. transmission by ticks not established. Emerging Infect Dis. 2010.
- Bai Y, et al. No evidence of Bartonella infections in host-seeking Ixodes scapularis and Ixodes pacificus ticks in the United States. Parasites & Vectors. 2024.
- Bai Y, et al. Bartonella infections are rare in blood-fed Ixodes scapularis and Ixodes pacificus ticks collected from rodents in the United States. Parasit Vectors. 2024.
- Edvinsson M, et al. Bartonella spp. seroprevalence in tick-exposed Swedish patients with persistent symptoms. Parasit Vectors. 2021.
- National Organization of Rare Disorders: Bartonellosis
- Medscape: Cat Scratch Disease (Cat Scratch Fever) Clinical Presentation
- Eikeland R. Tick-borne diseases in the North Sea region–A comprehensive overview and recommendations for diagnostics and treatment. 2024.
- Mazur-Melewska K, et al. Cat-scratch disease: a wide spectrum of clinical pictures. Postepy Dermatol Alergol. 2015.
- Mazur-Melewska K, et al. The significance of Bartonella henselae bacterias for oncological diagnosis in children. Infect Agents Cancer. 2015;10:30.
- Lins KA, et al. Cutaneous manifestations of bartonellosis. An Bras Dermatol. 2019.
- Massei F, et al. High prevalence of antibodies to Bartonella henselae among Italian children without evidence of cat scratch disease. Clin Infect Dis. 2004.
- Nelson CA, et al. Cat-Scratch Disease in the United States, 2005-2013. Emerging Infect Dis. 2016.
- Nelson CA, et al. Cat scratch disease: U.S. clinicians’ experience and knowledge. Zoonoses Public Health. 2018.
- Nawrocki CC, et al. Atypical Manifestations of Cat-Scratch Disease, United States, 2005–2014. Emerging Infectious Diseases. 2020
- Sander A, et al. Seroprevalence of antibodies to Bartonella henselae in patients with cat scratch disease and in healthy controls: evaluation and comparison of two commercial serological tests. Clin Diagn Lab Immunol. 1998..
- Boozalis E, et al. Demographic characteristics of teenage boys with horizontal striae distensae of the lower back. Pediatr Dermatol. 2018.
- Mada PK, et al. Bartonellosis StatPearls. StatPearls Publishing; 2018.
- Klotz SA, et al. Cat-scratch Disease. Am Fam Physician. 2011.
- Rolain JM, et al. Recommendations for treatment of human infections caused by Bartonella species. Antimicrob Agents Chemother. 2004.
- University of Guelph Worms and Germs blog: Cat Scratch Disease for Cat Owners
- LymeScience: Bartonella Rash vs Stretch Marks (a shorter version of this article)
- Philly Voice: Please don’t freak out about Cat Scratch Disease
- This Podcast Will Kill You: Bartonella: Keep Calm and Carrión 🔊
- Burk CJ, et al. Picture of the month. Striae. Arch Pediatr Adolesc Med. 2008.
Bartonella Quintana (trench fever caused by lice, not ticks)
- Boodman C, Gupta N, van Griensven J, Van Bortel W. Bartonella quintana detection among arthropods and their hosts: a systematic review and meta-analysis. Parasit Vectors. 2024.
- Rich SN, et al. Notes from the Field: Severe Bartonella quintana Infections Among Persons Experiencing Unsheltered Homelessness — New York City, January 2020–December 2022. MMWR Morb Mortal Wkly Rep. 2023.
- Keller M, et al. Bartonella quintana endocarditis in persons experiencing homelessness, New York, New York, USA, 2020–2023. Emerg Infect Dis. 2024.
- Louis S, et al. Perspectives of infectious disease physicians on Bartonella quintana cases, United States, 2014–2024. Emerg Infect Dis. 2024.
Cat-scratch Disease/Bartonella in Children
Kidshealth.org: Cat Scratch Disease
Childrens Hospital of Philadelphia: Cat Scratch Disease in Children
Amin O, et al. Cat Scratch Disease: 9 Years of Experience at a Pediatric Center, Open Forum Infectious Diseases. 2022.
Updated June 2, 2026